Gallbladder surgery recovery guide: Learn what to eat, what to avoid, and how to transition back to solid foods safely. Step-by-step diet advice to help your digestion adjust after cholecystectomy.
Undergoing a cholecystectomy (gallbladder removal) is a significant adjustment for your digestive system. While your body can function perfectly well without a gallbladder, you no longer have a “storage tank” for bile. Instead, bile flows continuously from your liver into your small intestine.
In the beginning, this can make digesting large amounts of fat or heavy meals a bit of a challenge. Learning what to eat and what to avoid can be the difference between a smooth recovery and uncomfortable digestive side effects.
Table of Contents
Why Your Diet Needs to Shift
The gallbladder’s primary job is to store and concentrate bile, which helps break down fats. Without it, bile is less concentrated. If you eat a high-fat meal shortly after surgery, your digestive tract might be overwhelmed, leading to bloating, gas, and “dumping syndrome” (rapid diarrhea).
The goal of a post-op diet isn’t just about restriction; it’s about retraining your digestive system to handle food in a new way.
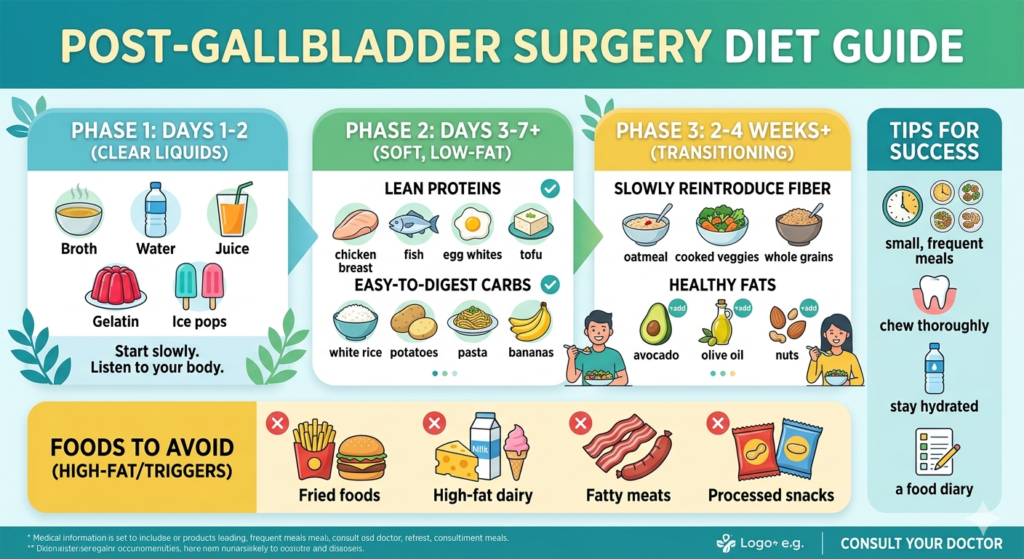
Phase 1: The First 24 to 48 Hours
Immediately following surgery, your surgeon will likely recommend a clear liquid diet. This ensures your bowels are waking up from anesthesia without being stressed.
- Broths: Chicken, vegetable, or beef bone broth (low sodium is best).
- Hydration: Water, herbal teas (ginger or peppermint are great for nausea), and electrolyte drinks.
- Light Sugars: Apple juice or white grape juice (avoid citrus or pulpy juices initially).
- Gelatin and Ice Pops: Simple, fruit-flavored gelatin or fruit juice popsicles.
Avoid carbonated drinks during this phase, as the gas used during laparoscopic surgery can already cause shoulder pain and bloating; bubbles will only add to the discomfort.
Phase 2: Introducing Soft, Low-Fat Foods
Once you can tolerate liquids, usually by day three or four, you can move toward soft solids. The “low-fat” rule is critical here. Aim for meals with less than 3 grams of fat per serving.
Lean Proteins
Protein is essential for tissue repair and healing. Stick to “white” meats and plant-based options:
- Boiled or Poached Chicken Breast: Skinless and prepared without oil.
- White Fish: Cod, tilapia, or pollock (baked or steamed).
- Egg Whites: Avoid the yolks initially, as they contain the fat.
- Tofu: A gentle, low-fat plant protein that is easy on the stomach.
Easy-to-Digest Carbohydrates
Carbs provide the energy needed for recovery. Focus on low-fiber options for the first week to prevent gas:
- White Rice or Pasta: Plain or with a tiny bit of salt.
- Toast or Crackers: Saltines or plain white toast.
- Mashed Potatoes: Prepare them with a little broth instead of butter or milk.
- Bananas: Part of the “BRAT” diet, they are easy on the gut and rich in potassium.
Phase 3: Transitioning to Long-Term Digestive Health
After the first week or two, you can begin slowly reintroducing more variety. This is the stage where you find your “new normal.”
The Importance of Fiber (Introduced Slowly)
While you avoid heavy fiber immediately after surgery, you eventually want it back in your diet to help normalize bowel movements. Fiber helps bulk up the stool and can prevent the diarrhea some people experience post-cholecystectomy.
- Oats and Oatmeal: Great for soluble fiber.
- Barley and Couscous: Heartier grains that are still relatively gentle.
- Cooked Vegetables: Carrots, zucchini, and green beans. Steaming them makes the cell walls easier to break down.
- Fruit (Peeled): Applesauce, pears, or peaches.
Healthy Fats (The “Drip” Method)
You don’t have to avoid fat forever. Your body still needs essential fatty acids for brain health and hormone production. The trick is portion control.
Try adding a teaspoon of olive oil or a small slice of avocado to a meal. If you feel fine, you can slowly increase the amount over several weeks.
Foods to Avoid (The “Caution” List)
Until your body has fully adjusted (which can take 4 to 8 weeks), these foods are the most likely to cause “bathroom emergencies” or cramping:
1. High-Fat and Fried Foods
Anything deep-fried, greasy, or cooked in heavy butter should be off the menu. This includes french fries, potato chips, and fried chicken.
2. High-Fat Dairy
Whole milk, heavy cream, full-fat cheeses, and ice cream are common triggers. If you crave dairy, opt for fat-free Greek yogurt or skim milk.
3. Fatty Meats
Avoid ribeye steaks, bacon, sausage, bologna, and dark meat poultry with the skin on. These require a “burst” of bile that you no longer have available.
4. Highly Processed Snacks
Store-bought cookies, cakes, and crackers often contain “hidden” fats like palm oil or butter that can irritate your system.
5. Spicy Foods
Capsaicin can speed up digestion. When combined with the continuous flow of bile, spicy peppers can lead to significant stomach upset and urgency.
Professional Tips for a Smooth Recovery
1. Eat Smaller, Frequent Meals
Instead of three large meals, aim for five or six small snacks throughout the day. This ensures that the constant trickle of bile from your liver is always “meeting” a small amount of food, rather than being overwhelmed by a large feast.
2. Keep a Food Diary
Every body reacts differently. Some people can eat pizza two weeks after surgery, while others struggle with eggs for months. Write down what you eat and how you feel two hours later. This helps you identify your personal “trigger foods.”
3. Chew Thoroughly and Eat Slowly
Digestion begins in the mouth. By breaking your food down mechanically as much as possible, you take the pressure off your small intestine.
4. Stay Hydrated
Bile is mostly water. Staying hydrated helps keep the bile fluid and moving, which can prevent the formation of stones in the bile duct a rare but possible post-surgery complication.
Sample One-Day Post-Op Menu
- Breakfast: Half a cup of oatmeal made with water, topped with half a sliced banana.
- Mid-Morning Snack: Two plain rice cakes or a few saltine crackers.
- Lunch: 3 oz of steamed cod with a side of white rice and well-cooked carrots.
- Afternoon Snack: Fat-free Greek yogurt or a cup of applesauce.
- Dinner: Poached chicken breast with a small baked potato (no skin, no butter) and steamed zucchini.
- Evening: A cup of peppermint tea.
When to Call Your Doctor
While some digestive upset is normal, keep an eye out for “red flag” symptoms that might indicate a complication like a bile leak or an infection:
- Severe abdominal pain that doesn’t improve with medication.
- Fever or chills.
- Yellowing of the skin or eyes (jaundice).
- Persistent vomiting or inability to keep liquids down.
- No bowel movement for more than three days post-surgery.
Final Thoughts
Recovery from gallbladder surgery is a marathon, not a sprint. Be patient with your body as it learns a new way to process nutrients. In a few months, most people find they can return to a relatively normal, healthy diet often feeling much better than they did before the surgery!




